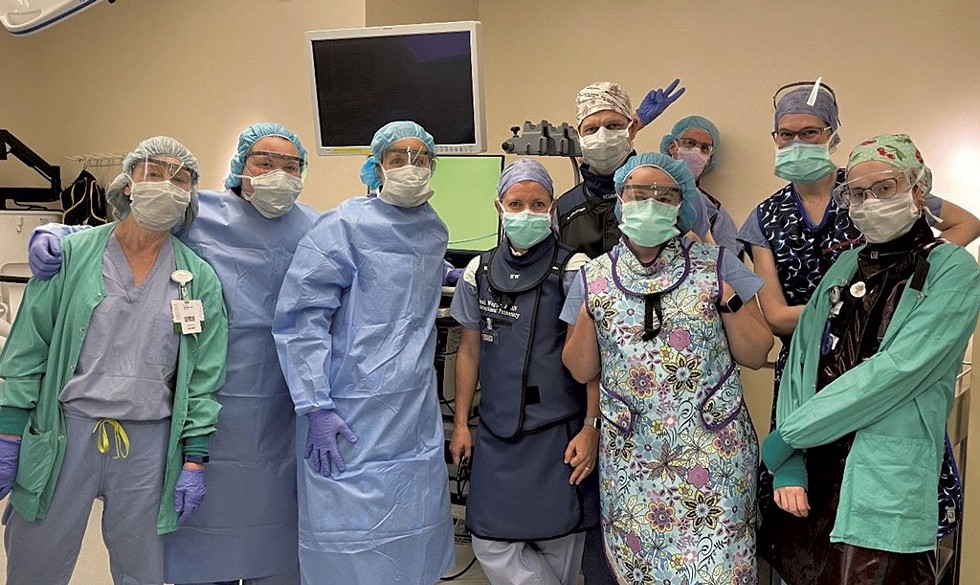
- Courtesy Photo
- Clinical trial operative team
How can we improve treatment for lung cancer? Dr. Matt Kinsey and a collaborative, multidisciplinary team at the University of Vermont Cancer Center are working on it.
Lung cancer is the deadliest form of cancer in the U.S.; it's not as common as skin, breast or prostate cancer, but it kills more people. It accounts for approximately 25 percent of cancer deaths around the country, according to the Centers for Disease Control and Prevention.
And lung cancer doesn't only affect smokers — Kinsey, who himself survived cancer as a child, points out that it's more common than pancreatic cancer in nonsmokers.
Now a doctor and Director of Interventional Pulmonary at the University of Vermont Medical Center, Kinsey is currently leading a clinical trial testing a new technique: delivering treatment directly to the tumor using a state-of-the-art robotic device. He's also working to make the process more efficient, so that clinicians can begin treating patients right away rather than waiting for a follow-up appointment weeks after a diagnosis.
This is research he wouldn't have thought possible just five years ago, Kinsey says. There have been major advances in his field over the last few years, particularly around immunotherapy, which harnesses the body's immune system to fight cancer.
"I think we are going to be able to immediately treat lung cancer at the time of diagnosis," he predicts. "We're going to be able to detect it and treat it, teach the body to kill it. That's the dream."
'The Way of the Future'
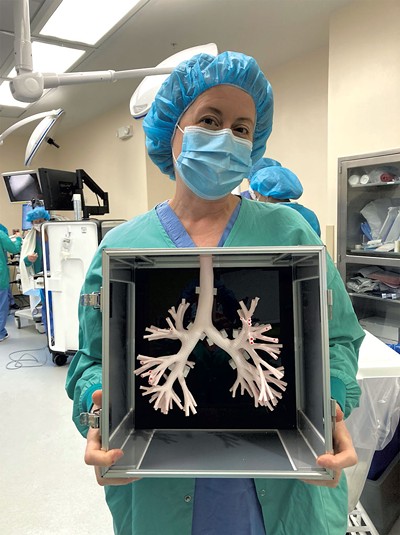
- Courtesy Photo
- Research coordinator Sarah Ardren
Currently, when people receive a lung cancer diagnosis, they set up an appointment with an oncology team that will help determine the course of treatment. That process can take a while.
It's awful to sit with the knowledge that you may have a deadly form of cancer and can't start fighting it for weeks. "The not-knowing is the hardest time," Kinsey says. "The more we can shorten that, the better."
It's particularly challenging for patients in outlying rural areas who have to drive two or three hours to an appointment at UVM Medical Center. Just arranging that transportation can take up valuable time. In theory, doctors could use the approach Kinsey is testing to initiate treatment immediately upon diagnosis.
Treatment for lung cancer often involves chemotherapy. Patients who undergo it receive powerful drugs intravenously that spread throughout the body — drugs that can cause serious side effects.
Kinsey and his team are studying whether injecting drugs directly into the tumor makes a difference, both in shrinking the cancer and diminishing the drug's side effects. They're using a robotic device to insert the needle into tumors that may be just over a centimeter in size. The machine is the only one of its kind in the Northeast outside of Boston, Kinsey notes. An intraoperative CT scanner is used to verify that the drugs are going directly into the tumor.
The approach "has a lot of intuitive appeal," Kinsey says. Patients may not be familiar with the phrase "intratumoral therapy," but they understand the concept and are eager to get the treatment. The U.S. Food & Drug Administration approved the trial; medical device and pharmaceutical company Johnson & Johnson is backing it.
"The Lung Cancer Initiative within Johnson & Johnson is funding the study because they believe delivering drugs directly into the tumors is the way of the future," Kinsey explains. The drug company doesn't have a financial interest in the drug currently being used, but it's hoping to use information gleaned from the study to develop drugs that can help patients in the years to come. "I think it's a great example of an academic-industry partnership, with the goal of moving an entire field forward," says Kinsey.
'So Willing to Collaborate'
Kinsey's trial is modest in size — just 10 to 20 patients. But it's exactly the kind of research that the Cancer Center is ideally suited to perform, he says.
The UVM Cancer Center is highly collaborative. In addition to Kinsey's staff from Interventional Pulmonary — Sarah Wagner, Brittany Hughes, Sara Ardren, Stephanie Burns, and a dedicated operating room nursing and respiratory therapy staff — the team behind these clinical trials also includes colleagues in Pathology (Drs. Kelly Butnor, Scott Anderson, and Pamela Gibson), Oncology (Drs. Farrah Khan and Peter Kaufman), Cardiothoracic Surgery (Dr. Mitch Norotsky), and Biostatistics (Dr. Chip Cole).
Kinsey's research group includes Dr. Emily DuComb, a pulmonary fellow who assists in running the clinical trial; Axel Masquelin, a graduate student performing quantitative image analytics; and Dr. Vitor Mori, who recently was awarded a highly competitive fellowship from the Damon Runyon Cancer Research Foundation to study intratumoral therapy for lung cancer.
Kinsey's mentor and collaborator, Dr. Jason Bates, works closely with Mori to evaluate distribution and kinetics of intratumoral drugs using computational models. Kinsey says he also feels very fortunate to work with Dr. Ralph Budd, whose lab — staffed by Cheryl Collins and Dolly Cupak — performs analyses of the immune cells within a tumor; and Dr. Jos van der Velden, who heads up UVM's Tumor Organoid Laboratory. Van der Velden grows cancer cells outside of patients to better understand how they respond to various interventions.
That's actually really difficult to do, Kinsey points out. Cancer is a problem because we can't stop it from growing in a human body. But researchers such as van der Velden have recently found a way to grow cancer cells in a lab.
It's quite a team. "We have so many people who are so skilled and so willing to collaborate," Kinsey says. "It's going to take all of these people to move the needle for patients."
'Impressed' by the Research

- Courtesy Photo
- Dr. Matt Kinsey
Kinsey's own bout with cancer played a role in determining his future. Diagnosed at age 8, he underwent almost two years of chemotherapy and had parts of both lungs resected. "The joke in high school was that I must have started smoking when I was a baby," he quips.
"There's a lot that goes into how you choose your career, and my experience is not something that gets written into residency or fellowship applications," he says, "but it is a big part of the reason I ended up doing what I do"
Kinsey grew up in Idaho and studied chemistry at the University of Idaho; he completed his medical doctorate — with distinction in research — at the Albert Einstein College of Medicine in the Bronx. After completing a Pulmonary and Critical Care Fellowship in the Harvard Combined Program, he pursued an additional year of training in Interventional Pulmonary at Massachusetts General Hospital/Beth Israel Deaconess Medical Center. He later earned a Master's in Public Health, with a focus in biostatistics, from the Harvard School of Public Health.
Kinsey had interviewed for fellowship training at the UVM Medical Center. "I was impressed by how much research was being done here," he says. He joined the Cancer Center, and the faculty of UVM's Larner College of Medicine, in 2013. His first impression proved correct. He's now one of more than 210 members of the Cancer Center, representing five UVM colleges, as well as the UVM Medical Center and Health Network.
Kinsey loves working with talented colleagues on cutting-edge research that could have a real, measurable effect on the lives of lung cancer patients. It's a unique opportunity the UVM Cancer Center offers, "and I'm honored to be part of it," he says. "For someone like me, it's fantastic."
About this series:
The University of Vermont Cancer Center in Burlington brings together research, medical education and state-of-the-art patient care, giving patients their best possible chance for survival. This 7D Brand Studio series, commissioned and paid for by Pomerleau Real Estate, explores some of the ways in which this extraordinary local resource benefits our community. Community donations support the exceptional research, education and care at the UVM Cancer Center. Please contact Lindsay at [email protected] for information.