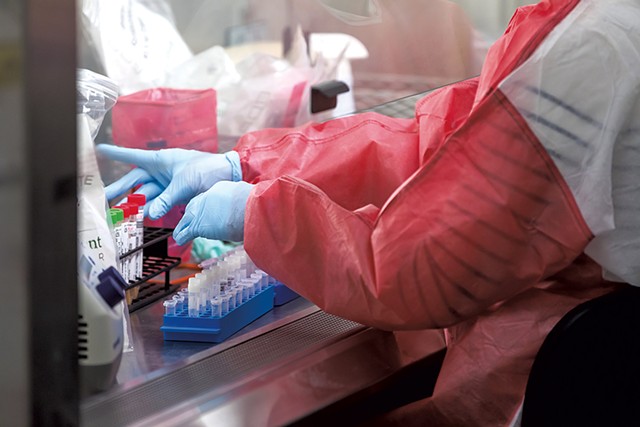
- File: Oliver Parini
- Running coronavirus tests at the Vermont Department of Health lab
Rapid-result antigen tests for COVID-19 are increasingly available at Vermont's nursing homes, urgent care clinics and private testing sites. Eldercare facilities, which are receiving testing equipment for free from the U.S. Department of Health and Human Services, have so far tested more than 700 people.
The Trump administration has heralded these rapid tests as a crucial tool in allowing states to reopen. But Vermont's guidelines strongly encourage the use of gold-standard PCR laboratory tests for the detection of the novel coronavirus — particularly in eldercare facilities. Antigen tests, the state says, should generally be used only on symptomatic people due to accuracy concerns.
Twenty-nine of Vermont's 35 nursing homes reported that they had received the antigen test machines. Fourteen of those homes have performed at least one test, and some have performed hundreds, according to data submitted on October 11 to the federal Centers for Medicare & Medicaid Services, which regulates nursing homes.
Vermont also has begun receiving shipments of an anticipated 180,000 antigen tests as part of a state-by-state mass distribution from the federal government, though local officials say they have not yet decided how they will use them.
The Vermont Department of Health favors PCR tests that detect the virus' genetic material in a sample, though the swabs must be analyzed in a lab and it can take a few hours to several days for results to be returned. Antigen tests, by contrast, detect proteins on the surface of the virus and can be performed in a matter of minutes using a tabletop or handheld diagnostic machine.
That speed is a big deal, said January Reichert, nursing director at Gill Odd Fellows Home of Vermont in Ludlow. The last time she PCR-tested all staff and residents, it took the lab five days to return the results. Two test results were inconclusive, forcing her to take those staffers out of the rotation for several days and retest them.
"It created a staffing issue, and it created a worry issue," she said.
Since then, Reichert said, the Broad Institute has promised quicker results. The state uses the private Massachusetts lab to handle routine testing for Vermont's nursing homes, and officials said the contract requires a 24-hour turnaround time for results once samples reach the lab. But Reichert said she's started using the antigen tests for additional screening of staff, as well as to test other workers who need to enter the home.
To test symptomatic residents, Reichert said, she uses the PCR tests instead.
The U.S. Food & Drug Administration gave emergency authorization for the first COVID-19 antigen test in May. Since then, it's authorized five other antigen tests. These tests have been vetted for their ability to detect the virus in patients experiencing symptoms within the first few days after onset.
But questions remain about their accuracy, particularly when given to asymptomatic people and in areas with low prevalence of the virus. The first test to win emergency approval from the FDA, made by San Diego-based Quidel, was at the center of a July incident in which 64 people tested positive at a Manchester, Vt., urgent care clinic. Follow-up PCR testing by the state Department of Health detected just four positive cases, and widespread testing found no evidence of an outbreak in the area.
That incident, as well as a similar one at a Maine summer camp, raised questions about reliability. Subsequent investigations by Quidel and the FDA found no issues with the tests or the Manchester clinic's procedures.
Vermont health officials have expressed concern about the use of antigen tests for diagnostic purposes. State officials don't count antigen test positives in daily case totals unless a laboratory test has confirmed the result.

- Andrea Suozzo
- Quidel Sofia 2 antigen test machine
And it's not just Vermont officials who have concerns. A national survey conducted by two eldercare industry groups and released in September found that 25 percent of the responding nursing homes had gotten at least one potential false-positive test result. Nevada health officials directed nursing homes to stop using the tests but rescinded the order after a threat of legal action from Health and Human Services.
Meanwhile, the Centers for Medicare & Medicaid Services published guidelines in late August that require routine testing of nursing home residents and staff using either PCR or antigen tests. The frequency depends on the disease prevalence in the surrounding community. Homes in the hardest-hit areas of the country must test twice weekly; Vermont homes must test just once a month.
In guidance about antigen tests released on October 1, Vermont health officials advised nursing homes and other providers to use PCR tests whenever available. The guidance suggested that antigen tests could be useful for rapid diagnosis of symptomatic patients but that they should not be used as a diagnostic tool in other scenarios. The tests could be used to monitor the members of a high-risk population — teachers or first responders, for instance — only if those tests were performed on a very frequent basis to track the prevalence of the virus in a group of people over time.
"If the clinical community uses them in an informed manner ... they can be very helpful tests in our overall management of this pandemic," Health Commissioner Mark Levine said at a news conference following the release of the guidance.
The state also informed homes that it expects to have the capacity to perform all the required tests via the PCR method through at least the end of December.
The day after the guidance came out, Pam Cota, licensing chief in the state's Division of Licensing and Protection, sent an email to nursing home administrators explaining that "it would not be a violation of testing requirements if your facility needed to use the antigen tests instead for the required testing," even though PCR tests are "clearly preferred" by state health officials.
Dr. Richard Feifer, chief medical officer at Genesis HealthCare, said the company's nine nursing homes in Vermont are all using PCR tests to fulfill federal testing requirements — but have also begun testing residents and staff using the antigen machines as a supplement. In a statement, Feifer said the rapid-result antigen tests can fill in the gaps when residents or staff "develop symptoms in between testing cycles."
At Wake Robin in Shelburne, health and resident services director Meagan Buckley said the facility's nursing home received an antigen test machine and 150 test kits in September but hasn't used them yet.
"We can and will utilize these antigen test kits should we need to in the future, but at this time we have been very pleased with our arrangements locally with [the University of Vermont Medical Center] for processing PCR tests," she said.
The extent of antigen testing being performed in Vermont is unclear.
At Gill Odd Fellows Home, Reichert said she's faxed records of the dozens of tests she's run to the Vermont Department of Health, as federal law requires. But the state is not reporting positive antigen test numbers publicly.
In fact, the health department said it's recorded only 90 antigen tests conducted in the state — and just one at a long-term-care facility. That's because the department only records positive results of those tests.
Still, antigen tests are becoming more widely available to the general public, not just to staffers and residents at long-term-care facilities. Earlier this month, Essex Junction-based Garnet Transport Medicine began offering both antigen tests and PCR tests at the Burlington International Airport. The service is available to travelers and members of the community. And ClearChoiceMD, an urgent care facility on Williston Road in South Burlington, offers the tests, as well.
A Seven Days staffer dropped by to request an antigen test last Friday. The clinic recommended a PCR test, as well, saying that method is more accurate. Two hours later, a worker swabbed the staffer twice in the parking lot. After fifteen minutes, she returned and handed over a piece of paper.
"Your Rapid COVID-19 test was negative," it read. "The test is roughly 86% accurate when negative, about 15% of negative test results will return positive when further testing is done, for this reason we sent out a nasal PCR COVID test for confirmation."
As tens of thousands of antigen test kits arrive from the federal government, it's unclear what the state will do with them. The Trump administration cited their potential usefulness in eldercare, K-12 schools and higher education. But Vermont has an existing PCR testing plan to cover long-term-care facilities, and the 180,000 antigen tests it will receive aren't sufficient to regularly test all public school students and staff. For now, the state does not have an immediate plan for the tests. At a press conference in early October, Levine described a cautious approach.
"We need to have a good understanding of their availability and their cost ... to be able to know how they fit in a long-term strategy," he said.
And since the federal government has not said whether it will send more of the tests once states have used the initial shipment, Levine said, "We'd hate to use the first set and then find that that strategy just ended because we no longer had access to them, either because of cost or because of manufacturing pipelines."














Comments
Comments are closed.
From 2014-2020, Seven Days allowed readers to comment on all stories posted on our website. While we've appreciated the suggestions and insights, right now Seven Days is prioritizing our core mission — producing high-quality, responsible local journalism — over moderating online debates between readers.
To criticize, correct or praise our reporting, please send us a letter to the editor or send us a tip. We’ll check it out and report the results.
Online comments may return when we have better tech tools for managing them. Thanks for reading.